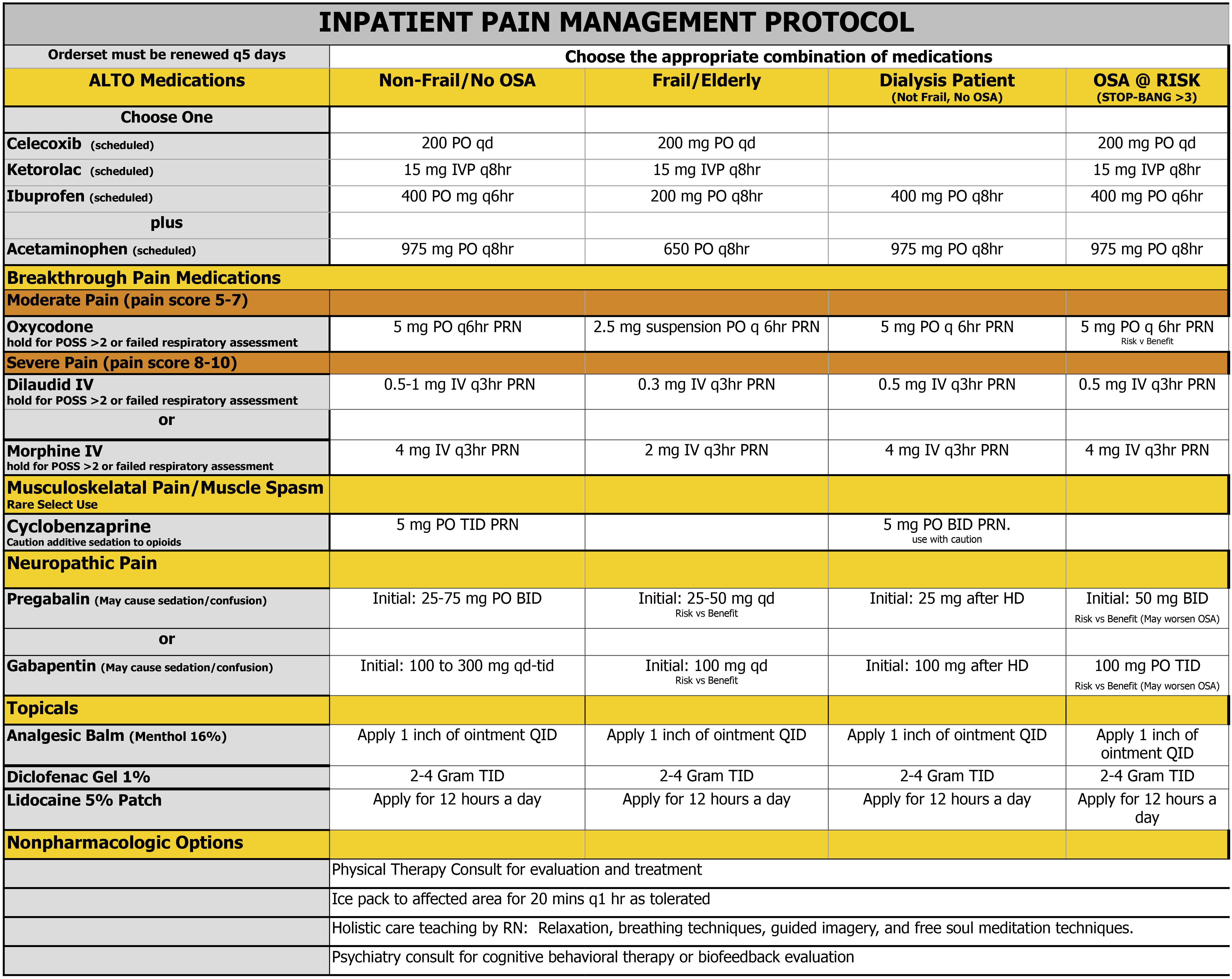
How pre-defined patient risk categories are transforming inpatient pain management programs
Chronic opioid use is the most common post-surgical complication — a poor long-term outcome that affects one in every 16 patients in the U.S. after surgery. Besides harming individuals and communities, excessive opioid prescriptions can also affect hospitals' profitability.
While multimodal pain programs attempt to reduce opioids, their “one size fits all” approach is inefficient for physicians and may cause sentinel events or adverse side effects that prolong a patient’s recovery.
This case study describes how a new inpatient pain management protocol using pre-defined patient risk categories yields meaningful clinical, operational, and financial
While multimodal pain programs attempt to reduce opioids, their “one size fits all” approach is inefficient for physicians and may cause sentinel events or adverse side effects that prolong a patient’s recovery.
This case study describes how a new inpatient pain management protocol using pre-defined patient risk categories yields meaningful clinical, operational, and financial
results.
Key learning points:
Key learning points:
- Why traditional multimodal pain programs that attempt to reduce opioids are inefficient
- The benefits of an updated inpatient pain management approach that relies on pre-defined patient risk categories
- How leveraging anesthesia expertise in this new approach to perioperative pain management saves time for busy hospitalists while improving patient safety and satisfaction
Please fill out the form to download the whitepaper